Direct Insurance Billing Software for Physio Clinics
Make physiotherapy affordable for your patients by collecting money directly from their insurance plans. Bill MSP, ICBC, WorkSafeBC, group benefit plans and patients in Claim Manager.
Want loyal patients?
Offer to submit their insurance claims.
Bill 15 insurers directly in one software
You will retain more patients when they are reimbursed for your service.
Only charge patients for the balance, if any
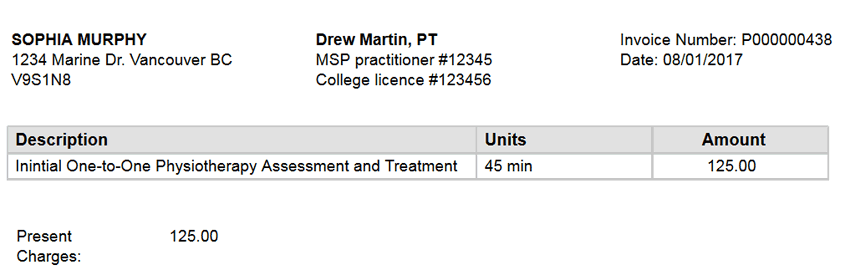
Create patient invoices that show the insurance benefits paid to your clinic.
See your clinic's revenues grow
Track your revenues daily with consolidated reports by all payees.
Insurers accepting electronic claims for physiotherapy
CINUP
Desjardins Insurance
Johnson
WorkSafeBC
Standard Life
First Canadian
Great West Life
Manulife
Maximum Benefit
Industrial Alliance
ICBC
Sun Life Financial
Cowan Insurance Group
MSP
Chambers of Commerce Group
Get software that makes your clinic profitable.
Bill insurers and the patient in three easy steps.
Collect $23 from MSP.
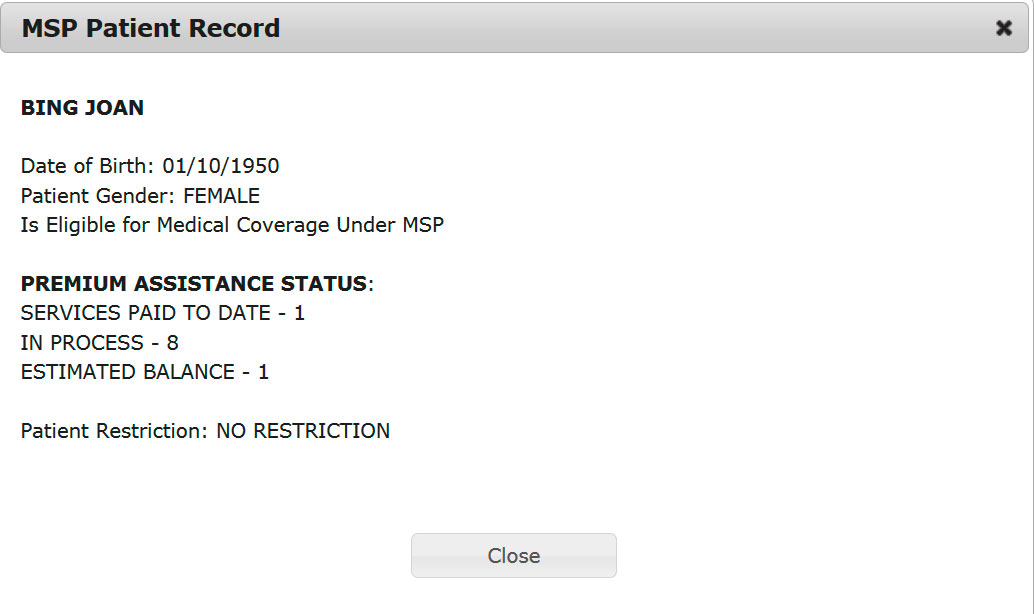
Check the balance of MSP visits and submit a physio claim for MSP Premium Assistance patient.
Collect benefits from extended health.
If physiotherapy is covered by the patient’s group benefit plan, bill the plan for the fee remainder.
Collect fee balance, if any, from the patient.
If the insurance benefits do not cover your fee, invoice the patient for the balance.
You can bill MSP, a group benefit plan and the patient in one transaction
and have your billing done quicker.
All billing scenarios for your physio clinic
Submit a claim to MSP, ICBC, WorkSafeBC or a group benefit plan and invoice the patient for the balance, if any.
UNINSURED PATIENT
Invoice the patient for full amount if no healthcare benefits are available.
Invoice patients quicker
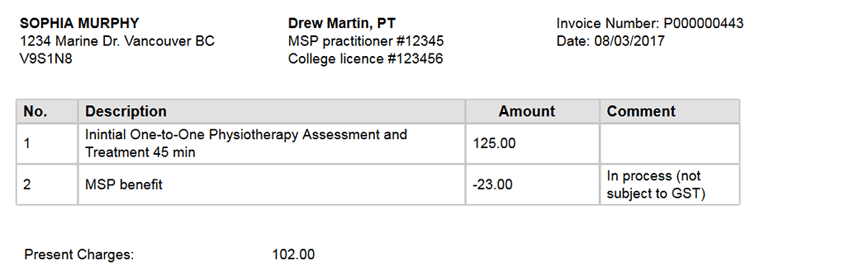
PATIENT INSURED BY MSP
Bill $23 to MSP and collect the rest from the patient.
The easiest way to bill MSP
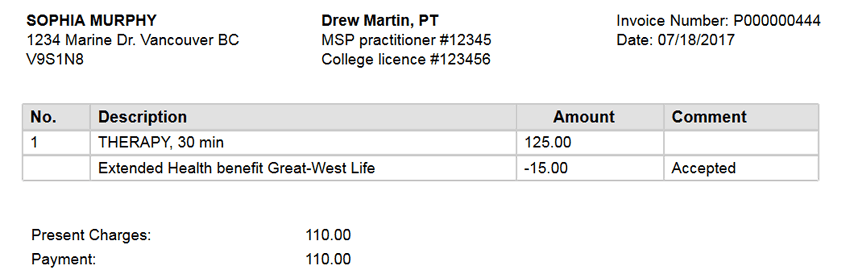
INSURED BY A GROUP BENEFIT PLAN
Bill service to the group benefit plan and balance to the patient.
Real-time adjudication*
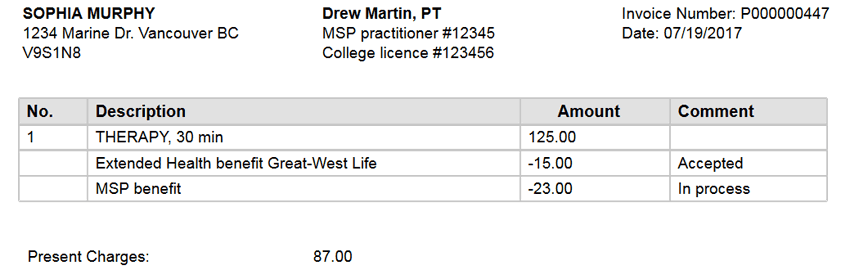
MSP + GROUP BENEFITS
Bill $23 to MSP and balance to group benefits and the patient.
make all plans count
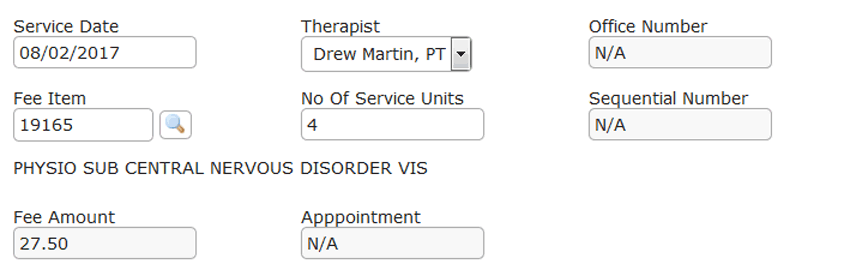
INSURED BY ICBC
Do not reject ICBC patients.
1. Collect payments from ICBC
Get paid directly by ICBC at ICBC rate.
2. Bill ICBC surcharge to patients
Invoice the patient for the balance when ICBC benefits less than your fee.
3. Help patient collect the user fee from a group benefit plan
After invoicing patient, offer to submit a claim on the patient’s behalf.**
** When allowed by the insurer.
INSURED BY WORKSAFEBC
Collect money from WorkSafeBC for insured patients.
Submit fee-for-service invoices
True patients’ loyalty starts with Claim Manager
Add additional value to your life-changing treatment.
Instant price relief
Ensure that your patient gets an instant price discount in the form of the insurance benefits.
No billing headache
Don’t make your patients go through laborious insurance paperwork. Submit their claims with ease.
Benefits check
Many patients don’t know about their benefits. Check their eligibility and help plan their health care budget.*
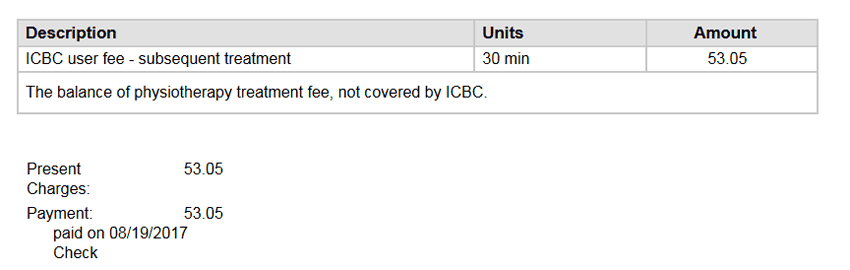
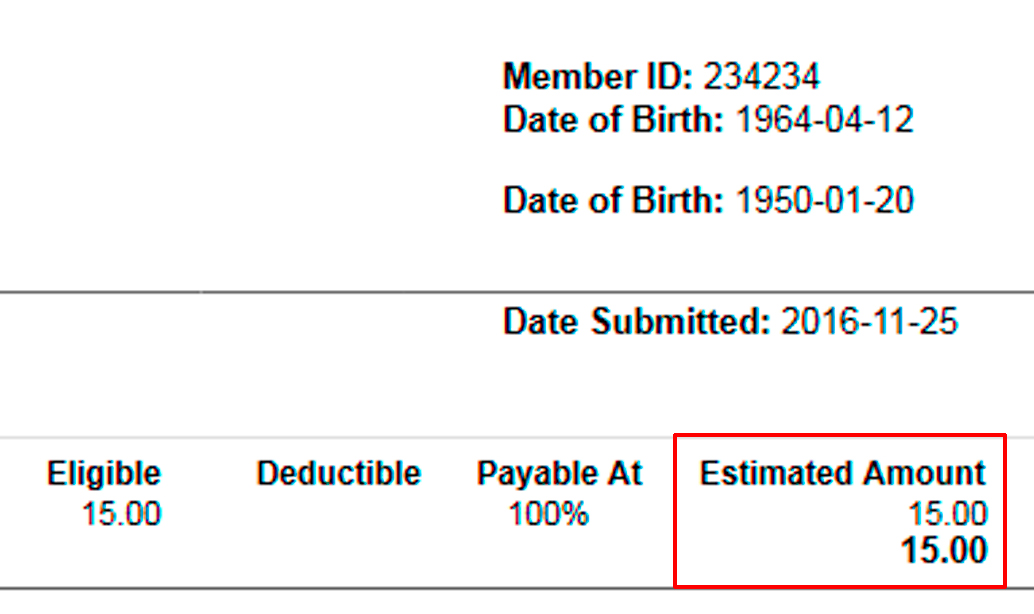
Explanation of benefits for physio claims
An Explanation of Benefits is the adjudication response to your insurance claims that shows how much will be paid.
Create invoices that account for all benefits paid to your clinic
and have us do the math.
Try it today. Limited time offer.
Claim Manager helps you comply with insurance rules
Are you aware of the mandatory forms that you have to keep on file for your patients? Claim Manager fills them out and reminds you when you need to have them signed.
MSP billing compliance
Pre-filled Assignment of MSP Benefits form for patients insured by MSP
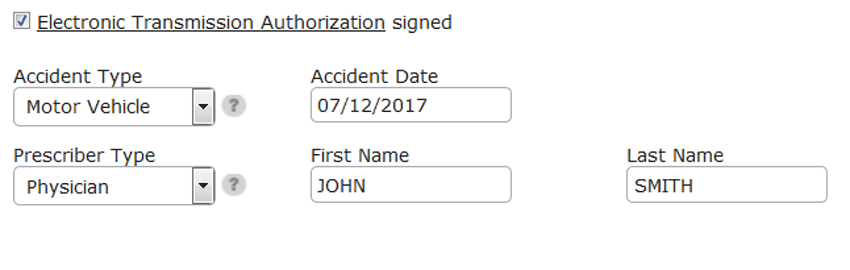
Group benefits compliance
Pre-filled Electronic Transmission Authorization (ETA) and Benefits Assignment (BA) forms
Did you know that you are supposed to bill MSP before private insurance plan?
Claim Manager will check MSP coverage and account for MSP benefit when billing the private insurance plan.
3 reasons to transfer your billing to Claim Manager
Enter data once
Don’t enter same data into two software. Use Claim Manager for everything.
Consolidate reports
Keep all your records in one place and prepare all kinds of reports quickly.
Bill all payees at once
Bill the visit to multiple payees in one go. Show all benefits on one invoice.
Try it today. Limited time offer.